Lumbar disc herniation is one of the most common spinal conditions affecting millions of people worldwide, causing debilitating lower back pain that can radiate down the legs. This condition doesn't just impact physical health; its effects extend to quality of life, work capacity, and the ability to perform everyday activities.
Understanding the nature of lumbar disc herniation, its causes, and symptoms represents the first step toward effective treatment. With significant medical advances, there are now multiple treatment options ranging from simple conservative therapies to advanced surgical interventions, giving patients a better chance at recovery and returning to normal life.
In this comprehensive guide, we will explore in detail everything related to lumbar disc herniation, from diagnosis to the latest treatment and prevention methods. At Safemedigo, we are committed to providing you with accurate and reliable information to help you make the right decision about your health.
Understanding Lumbar Disc Herniation
To properly understand lumbar disc herniation, you must first know how the spine and the intervertebral discs that separate the vertebrae work.
What is a lumbar disc herniation?
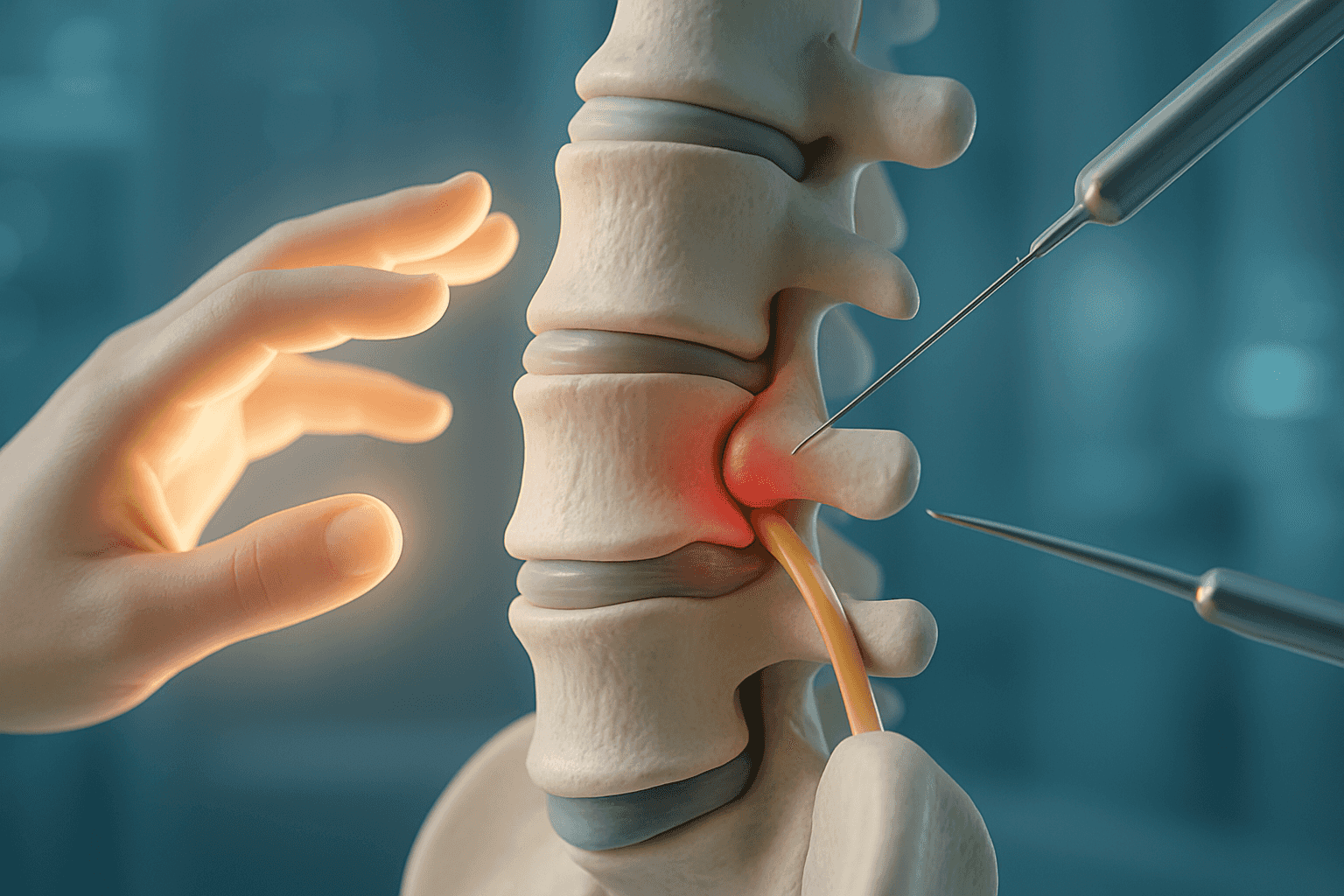
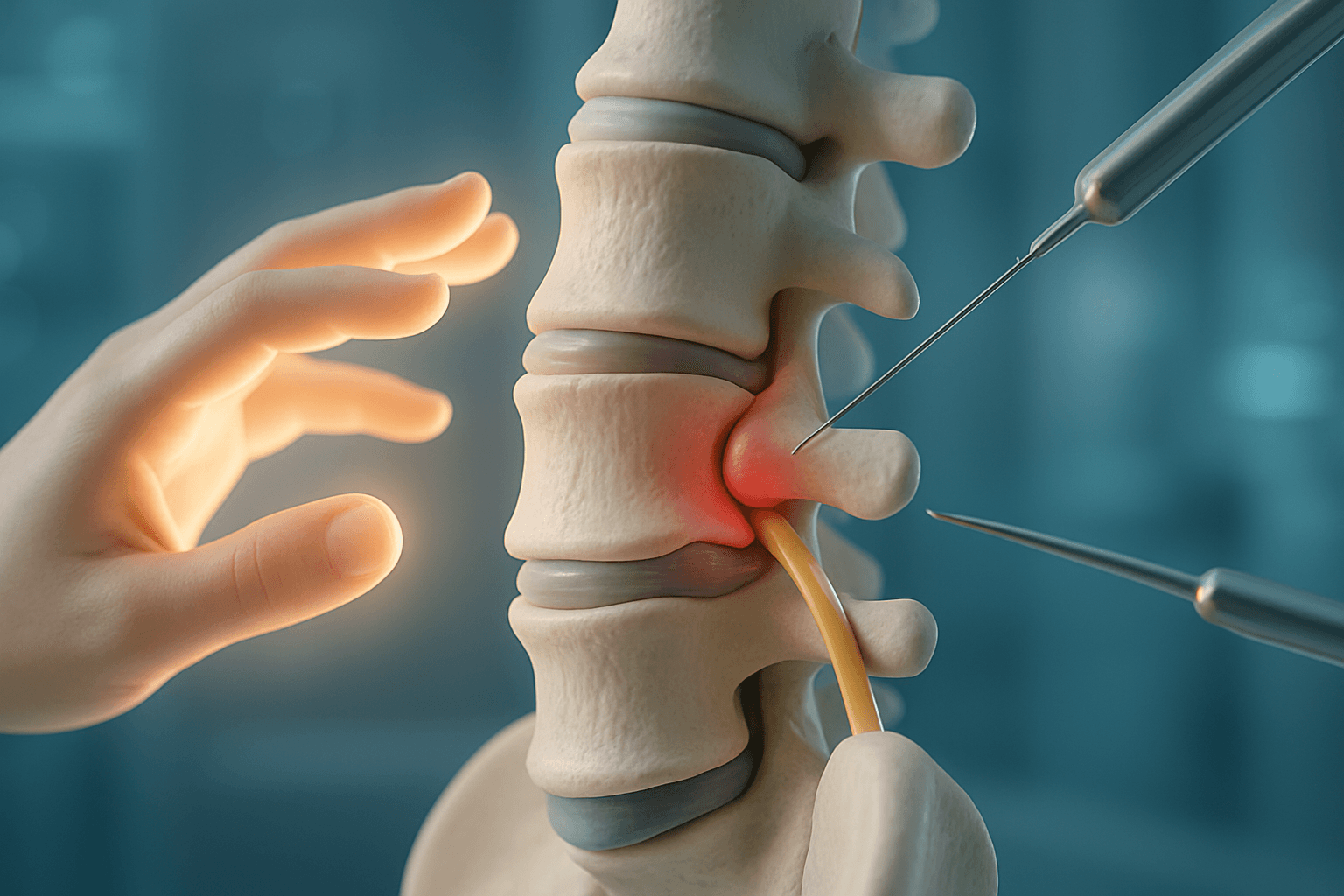
A lumbar disc herniation is a medical condition that occurs when the intervertebral disc located between the vertebrae in the lower back tears or slips. These discs act as shock-absorbing cushions between the vertebrae and consist of a tough outer part called the annulus fibrosus and a gel-like inner part called the nucleus pulposus.
When a tear occurs in the outer ring, the inner gel-like material can push outward, leading to pressure on the adjacent nerves. This pressure is the main cause of pain and other symptoms associated with lumbar disc herniation.
The lumbar region of the spine consists of five vertebrae that bear the greatest amount of body weight, making them more susceptible to disc herniation. The fourth and fifth lumbar vertebrae are most commonly affected by this condition.
How does a lumbar disc herniation occur?
Lumbar disc herniation occurs due to several factors that may work alone or together. The primary factor is the natural wear and tear of the intervertebral discs with aging, as these discs gradually lose their water content, making them less flexible and more prone to tearing.
Sudden or incorrect movements play a major role in causing disc herniation. Lifting heavy objects incorrectly, especially while twisting at the same time, can place tremendous pressure on the intervertebral discs. Similarly, a sudden fall or exposure to a strong impact on the back area may lead to disc rupture.
Sitting for long periods in incorrect postures, especially in desk work or long-distance driving, increases pressure on the lumbar vertebrae. Excess weight places an additional burden on the spine, accelerating the wear and tear process of the intervertebral discs.
Who is at risk of lumbar disc herniation?
Some groups are more susceptible to lumbar disc herniation than others. People aged between 30 and 50 years are most affected, as the intervertebral discs begin to lose their natural flexibility during this age range.
Workers in occupations that require frequent lifting of heavy loads, such as construction and transportation workers, are at greater risk. Likewise, people suffering from obesity face an increased risk due to additional pressure on the spine.
Genetic factors also play a role, as some people inherit weakness in the structure of the intervertebral discs. Smokers are also more susceptible to injury, as smoking reduces blood flow to the intervertebral discs, accelerating their deterioration.
Symptoms of Lumbar Disc Herniation
The symptoms of lumbar disc herniation vary from person to person depending on the location of the herniation and the degree of pressure on the nerves.
Recognising symptoms of lumbar disc herniation
Lower back pain is the most common symptom of lumbar disc herniation. This pain may be acute and sudden or may develop gradually over days or weeks. The pain usually increases with movement, especially when bending, twisting, or lifting objects.
Leg pain, medically known as sciatica, is a distinctive sign of lumbar disc herniation. This pain occurs when the herniated disc presses on the sciatic nerve, causing sharp pain that extends from the lower back through the buttocks to the lower leg, and may reach the foot.
Numbness and tingling in the leg or foot are also common symptoms. The patient may feel a sensation similar to pins and needles or partial loss of sensation in the areas supplied by the compressed nerve. Muscle weakness in the affected leg may make it difficult to walk or stand on tiptoes or lift the foot.
When leg pain and sciatica signal a lumbar disc herniation
Not all leg pain necessarily means there is a disc herniation, but there are certain characteristics that indicate that lumbar disc herniation and sciatica are related. If the pain starts in the lower back and then spreads to the buttocks and leg, this is a strong indicator of disc herniation.
Pain that worsens when sitting, coughing, sneezing, or laughing indicates nerve compression. If the pain follows a specific path along the back or side of the leg, this is consistent with the distribution of the sciatic nerve.
In more severe cases, sciatic nerve pain may be accompanied by noticeable weakness in the leg or foot muscles. The patient may find it difficult to lift the foot off the ground while walking, a condition known as foot drop.
Red flags requiring urgent care for lumbar disc herniation
Some symptoms require immediate medical attention because they may indicate a serious condition called cauda equina syndrome. This rare but serious condition occurs when severe disc herniation compresses the bundle of nerves at the end of the spinal cord.
Loss of bladder or bowel control is the most serious sign and requires emergency surgical intervention. Numbness in the saddle area, which is the area that touches the saddle when riding a horse, also indicates severe nerve compression.
Progressive weakness in the legs, especially if it affects both legs, warrants urgent medical evaluation. Severe pain that does not respond to regular painkillers or that progressively worsens should prompt you to seek medical help.
Read about: Lumbar spinal fusion
Diagnosing Lumbar Disc Herniation
Accurate diagnosis of lumbar disc herniation is the key to developing an effective treatment plan.
Role of MRI and imaging in lumbar disc herniation
Magnetic resonance imaging is considered the gold standard test for diagnosing lumbar disc herniation. MRI provides detailed images of soft tissues, including intervertebral discs, nerves, and the spinal cord.
Through MRI, the doctor can accurately see the location of the herniation, determine the size of the herniated disc material, and assess the extent of nerve compression. This examination does not use harmful radiation, making it safe for repeated use if necessary.
MRI also helps rule out other conditions that may cause similar symptoms, such as tumors, infections, or spinal stenosis. The results guide the doctor in choosing the most appropriate treatment, whether conservative or surgical.
Clinical tests and diagnosis of lumbar disc herniation
Before resorting to advanced imaging, the doctor begins with a comprehensive clinical examination. This examination includes assessing the range of motion of the back, testing nerve reflexes, and measuring muscle strength in the legs.
The straight leg raise test is a classic examination used to assess disc herniation. The doctor asks the patient to lie on their back and then slowly raises their straight leg. If this causes sharp leg pain before reaching a 60-degree angle, this strongly indicates disc herniation.
X-rays may be useful to rule out bone problems such as fractures or arthritis, but they do not clearly show the intervertebral discs. Computed tomography can provide more detail about bones and discs, but it is less accurate than MRI in imaging soft tissues.
Assessing severity and levels of lumbar disc herniation
Lumbar disc herniation is classified into several grades according to its severity. Mild lumbar disc herniation occurs when there is a slight bulge in the disc without a complete tear in the outer ring. This type may cause mild symptoms and responds well to conservative treatment.
Disc protrusion is the next stage, where the disc begins to move out of its position but the gel-like material is still contained within the outer ring. Complete herniation occurs when the outer ring tears and the gel-like material exits.
Severe lumbar disc herniation is the most serious, where a piece of the gel-like material may completely separate and move into the spinal canal. This type causes severe symptoms and may require urgent surgical intervention.
Non-Surgical Treatments for Lumbar Disc Herniation
The vast majority of lumbar disc herniation cases improve with conservative treatment without the need for surgery.
Conservative management of lumbar disc herniation
Rest in the first few days after symptoms appear is important, but complete rest for long periods may be harmful. Relative rest for only a day or two is recommended, then gradual return to light activities.
Modifying daily activities means avoiding movements that increase pain, such as forward bending, lifting heavy objects, or sitting for long periods. Using a small pillow under the lower back when sitting can help maintain the natural curve of the spine.
Applying ice to the affected area in the first few days helps reduce inflammation and pain. After 48 hours, you can switch to moist heat which helps relax muscles and improve blood flow.
Exercises for lumbar disc herniation
Exercises for lumbar disc herniation play a crucial role in treatment and prevention. These exercises aim to strengthen the back and abdominal muscles, improve flexibility, and reduce pressure on the intervertebral discs.
Gentle stretching exercises for the spine help relieve pressure on the nerves. The knee-to-chest exercise, where the patient lies on their back and pulls one knee toward their chest, helps stretch the lower back muscles.
Abdominal muscle strengthening exercises are important because these muscles support the spine from the front. Modified plank exercises and bridge exercises strengthen these muscles without placing excessive pressure on the back.
Recommended exercises for lumbar disc herniation should be performed under the supervision of a physical therapist, especially initially. Incorrect exercises may worsen the condition instead of improving it.
Support braces and lumbar disc herniation rehabilitation
A back brace for lumbar disc herniation may be useful in some cases, especially during activities that place stress on the back. The brace provides external support to the spine and reminds the patient to maintain a healthy posture.
However, the brace should be used with caution and for limited periods. Excessive reliance on the brace may lead to weakening of the natural back muscles. It is preferable to use it only when performing certain activities and then remove it.
Stretching the lower back muscles after disc herniation is an important part of treatment. Regular stretching exercises maintain muscle flexibility and prevent spasms. Therapeutic massage may also help relieve muscle tension.
Read about: Endoscopic Spine Surgery: Safety and Key Advantages
Medical and Injection Options for Lumbar Disc Herniation
Medications and injections play an important role in controlling pain and inflammation associated with disc herniation.
Medications for lumbar disc herniation pain relief
Non-steroidal anti-inflammatory drugs are the first line in treating lumbar disc herniation. These medications not only relieve pain but also reduce inflammation around the compressed nerve.
Simple painkillers may be sufficient for mild cases. In more severe cases, the doctor may prescribe stronger painkillers or muscle relaxants to relieve accompanying muscle spasms.
Nerve medications may be effective in treating sciatic nerve pain. These medications work to calm irritated nerves and reduce pain resulting from nerve compression.
Injections for lumbar disc herniation: when why
Injections for lumbar disc herniation are used when oral medications are not sufficient to control pain. Epidural cortisone injections are the most common, where a powerful anti-inflammatory medication is injected directly around the compressed nerve.
These injections can provide significant pain relief for a period ranging from weeks to months. The main benefit is that they allow the patient to participate more effectively in physical therapy and rehabilitation exercises.
Injections are not a final cure for disc herniation, but rather a means of controlling symptoms. Some patients may need repeated injections, but it is preferable not to exceed three injections per year to avoid potential side effects of cortisone.
When non-surgical treatment fails: considering surgery for lumbar disc herniation
Medical treatment is considered to have failed if severe pain continues for more than 6 to 12 weeks despite full adherence to conservative treatment. If the pain significantly impairs the patient's ability to work or perform basic daily activities, it may be time to consider surgical options.
Progressive muscle weakness is an important indicator of the need for surgical intervention. If the patient notices that their leg muscles are continuously weakening, this means that the pressure on the nerve is causing damage that may become permanent if not treated.
Loss of bladder or bowel control, as mentioned earlier, is an emergency requiring immediate surgery. In this case, there is no time to try conservative treatments.
Read about: Chronic Disc Herniation: When Is Surgical Intervention Needed?
Surgical Treatment for Lumbar Disc Herniation
When conservative treatment fails, surgery becomes a necessary option to relieve pressure on the nerves and restore normal function.
Indications for lumbar disc herniation surgery
Surgery for lumbar disc herniation is used in specific cases. The most common case is the failure of conservative treatment to relieve pain after a sufficient trial period, usually 6 to 12 weeks.
Progressive neurological weakness is a strong indicator for surgery. If the patient is increasingly losing the ability to move their foot or toes, surgery may be necessary to prevent permanent damage.
Cauda equina syndrome, as mentioned, is an emergency requiring immediate surgery within 48 hours to avoid permanent nerve damage. Severe unbearable pain that does not respond to any other treatment may also be a justification for surgery.
Types of surgery and minimally invasive options
Microdiscectomy is the most common type of lumbar disc herniation surgery. In this procedure, the surgeon uses a surgical microscope to remove the herniated portion of the disc that is pressing on the nerve. The surgery is performed through a small incision, reducing damage to surrounding tissues.
Endoscopic discectomy is a less invasive technique, where precise surgical instruments are inserted through a very small incision. This technique results in less post-operative pain and faster recovery, but it may not be suitable for all cases.
In some more complex cases, the surgeon may need to remove the entire disc and fuse the adjacent vertebrae. This procedure, known as spinal fusion, is used when there is instability in the spine or when simpler surgeries fail.
Read about: Herniated Disc Surgery: When Is It Necessary? Full Recovery Guide
Recovery and outcomes after lumbar disc herniation surgery
Most patients notice immediate improvement in leg pain after lumbar disc herniation surgery. Back pain may take longer to improve. Patients can usually walk on the same day of surgery or the next day.
The complete recovery period usually ranges from 4 to 6 weeks for simple surgeries. During this period, lifting heavy objects and excessive bending should be avoided. Physical therapy usually begins two weeks after surgery.
The success rate of lumbar disc herniation surgery is high, with about 85-90% of patients experiencing significant improvement in symptoms. However, there is a small risk of recurrence of herniation in the same place or elsewhere in the future.
Rehabilitation Exercise Post-Lumbar Disc Herniation
Physical therapy and regular exercise are the cornerstone of recovery from disc herniation and prevention of recurrence.
Recommended exercises after a lumbar disc herniation
Exercises after lumbar disc herniation should be gradual and supervised by a specialist. In the acute phase, gentle stretching exercises are most appropriate. The pelvic tilt exercise, where the patient lies on their back and tightens the abdominal muscles to flatten the lower back on the floor, helps strengthen the core muscles.
The cat-cow exercise, where the patient is on all fours and gently arches their back up and down, improves spinal flexibility. The bridge exercise, where the patient lies on their back with knees bent and then lifts the buttocks off the floor, strengthens the back and buttock muscles.
As the condition improves, more challenging exercises can be added such as side plank exercises and balance exercises. Swimming and water walking are excellent exercises because they strengthen muscles without placing great pressure on the spine.
Strengthening the back and preventing the recurrence of lumbar disc herniation
Pain management after treatment requires a multifaceted approach. Maintaining regular moderate physical activity helps prevent muscle stiffness and reduce pain. Avoiding sitting or standing for long periods without changing position is also important.
Relaxation techniques such as deep breathing and meditation may help reduce muscle tension and chronic pain. Heat or cold therapy can be used as needed to relieve pain.
Strengthening the core muscles, including the abdominal, back, and buttock muscles, provides better support for the spine and reduces the risk of recurrent injury. A regular exercise program that continues for life is the best investment in your back health.
Managing mild lumbar disc herniation without surgery
Mild lumbar disc herniation often improves spontaneously with time and conservative treatment. The body has a natural ability to gradually absorb the herniated disc material, especially in mild cases.
Lumbar disc herniation without surgery can be successfully treated in most cases through a combination of moderate rest, medications, physical therapy, and regular exercise. Patience is important, as improvement may take several weeks to months.
Full and continuous adherence to conservative treatment is the key to success. Many patients stop physical therapy as soon as they feel a slight improvement, which increases the risk of symptoms returning.
Prevention Lifestyle After Lumbar Disc Herniation
Preventing lumbar disc herniation or preventing its recurrence requires changes in lifestyle and daily habits.
Preventive strategies for lumbar disc herniation
Preventive strategies for lumbar disc herniation focus on maintaining a healthy weight and providing the necessary nutrients for spinal health. Excess weight places additional pressure on the intervertebral discs, so maintaining an ideal weight is the most important dietary factor.
Foods rich in anti-inflammatory properties such as fatty fish, nuts, colorful fruits and vegetables help reduce inflammation in the body. Calcium and vitamin D are important for bone health and can be obtained from dairy products, fish, and moderate sun exposure.
Adequate hydration is very important for the health of the intervertebral discs. These discs contain a high percentage of water, and dehydration can accelerate their deterioration. Drinking at least 8 glasses of water daily helps maintain disc flexibility.
Lifestyle habits to protect your lumbar spine
Proper body mechanics are essential for prevention. When lifting, always bend from your knees, not from your waist. Keep your back straight and hold the object close to your body. Avoid twisting while lifting.
When sitting, sit with your back straight and shoulders back. Your knees should be slightly lower than your hips. Use a lumbar support if needed. Avoid sitting for prolonged periods; get up and stretch every 30 minutes.
When sleeping, sleep on a medium-firm mattress. Sleeping on your side with a pillow between your knees or on your back with a pillow under your knees helps maintain the natural curve of the spine.
When to use support devices or ergonomic adjustments for lumbar disc herniation
A back brace may be useful for short periods when performing activities you know will strain your back. However, do not rely on it permanently as this may weaken your natural back muscles.
If your job is physically demanding, you may need to discuss modifications with your employer, such as using ergonomic equipment or alternating tasks to avoid repetitive strain. In some cases, a career change may be necessary to protect your back in the long term.
Using assistive tools such as hand carts to transport heavy objects, ergonomic office chairs can significantly reduce pressure on the spine.
Read about: Is Spine Surgery Safe? Recovery Stages and Post-Op Care
When and Where to Seek Help for Lumbar Disc Herniation
Knowing when to seek specialized medical help is crucial to preventing long-term complications.
Warning signs of serious lumbar disc herniation
As mentioned earlier, any signs of cauda equina syndrome (loss of bladder or bowel control, saddle numbness) require an immediate trip to the emergency room. You should also see a doctor promptly if you have progressive leg weakness or if your pain is severe and not improving with self-care.
If the pain is severe and does not improve with self-care within a week, or if it is progressively worsening, you should consult a doctor. Pain accompanied by fever or unexplained weight loss may indicate a more serious condition.
If the pain significantly affects your ability to work, sleep, or perform basic daily activities, it may be time to seek specialized help.
Choosing a spine specialist for lumbar disc herniation
If your back pain persists, your primary care doctor will likely refer you to a specialist. This could be a physiatrist (a physical medicine and rehabilitation doctor), a pain management specialist, a neurosurgeon, or an orthopedic spine surgeon.
For non-surgical management, a physiatrist is often a good starting point. If surgery is being considered, you should consult with an experienced spine surgeon. If you are looking for expert advice, the specialists at Safemedigo can provide a comprehensive evaluation and guide you to the best treatment option.
Recovery timeline: how long does lumbar disc herniation treatment last?
The duration of treatment for lumbar disc herniation varies greatly. For many people, symptoms will significantly improve within 6 weeks with conservative care. For others, it may take several months.
The cost also varies depending on the treatments needed. Physical therapy, injections, and surgery all have different costs, which can also vary by location and insurance coverage. It is important to have a clear discussion with your healthcare provider about the expected timeline and costs.
Conclusion
Lumbar disc herniation can be a painful and frustrating condition, but it is important to remember that the outlook is generally very positive. The vast majority of patients find relief with conservative treatments like physical therapy and lifestyle modifications.
For the small percentage who do require surgery, modern minimally invasive techniques offer excellent results with a rapid recovery. The key to a successful outcome is an accurate diagnosis, a personalized treatment plan, and an active partnership between you and your healthcare team.
By taking an active role in your recovery and adopting a back-healthy lifestyle, you can not only overcome your current symptoms but also significantly reduce your risk of future problems. Don't let back pain dictate the terms of your life. Are you ready to find a lasting solution? Contact the expert team at Safemedigo via WhatsApp today for a comprehensive evaluation and to discuss the best treatment options for your specific condition. We are here to support you on your journey back to an active, pain-free life.
Frequently Asked Questions: Lumbar Disc Herniation
Can a herniated disc heal on its own?
Yes, in many cases it can. The body's immune system can recognize the herniated disc material as a foreign substance and attack it, causing it to shrink over time. Also, some of the water content of the herniated portion can be reabsorbed by the body, reducing its size. This process, combined with a reduction in inflammation, can lead to a significant improvement in symptoms over several weeks to months.
Is walking good for a herniated disc?
Yes, gentle walking is generally one of the best activities for a herniated disc. It helps to increase blood flow to the spine, which promotes healing, and it can help reduce stiffness and prevent muscle deconditioning. It is important to start slowly, listen to your body, and avoid walking on hard or uneven surfaces. If walking causes a significant increase in your pain, you should stop and consult your doctor or physical therapist.
What should I avoid if I have a herniated disc?
You should avoid activities that put a lot of stress on your lower back. This includes heavy lifting, bending forward from the waist, prolonged sitting (especially in a slouched position), and high-impact activities like running or jumping. You should also avoid any specific movement or position that consistently makes your leg pain worse.
How long does the pain from a herniated disc last?
The duration of pain varies widely. For an acute herniation, the most severe pain often lasts for a few days to a couple of weeks. With conservative treatment, most people see a significant improvement within 6 to 12 weeks. However, some people may experience chronic or intermittent pain for a longer period.
Will I need surgery for my herniated disc?
Probably not. Over 90% of people with a lumbar disc herniation get better with non-surgical treatment. Surgery is only considered if you have emergency symptoms (cauda equina syndrome), progressive muscle weakness, or severe, disabling pain that does not improve after a full course of conservative care.