A herniated disc is one of the most common spinal conditions, affecting thousands of people every year. If you're experiencing back or neck pain, numbness, or muscle weakness in your limbs, you may be suffering from a herniated disc.
But the most critical question is: When is herniated disc surgery necessary? And what are the symptoms requiring herniated disc surgery?
In this comprehensive guide, we’ll explore:
- What is a herniated disc?
- The difference between lumbar disc herniation surgery and cervical disc herniation surgery
- Herniated disc surgical indications
- Herniated disc surgery vs conservative treatment
- Minimally invasive herniated disc surgery options
- Herniated disc surgery recovery timeline
- And much more, including post-surgery rehabilitation and recovery exercises
Let’s dive into the full picture of when surgery is needed — and what to expect during recovery.
What Is a Herniated Disc?
Difference Between Lumbar Disc Herniation Surgery and Cervical Disc Herniation Surgery
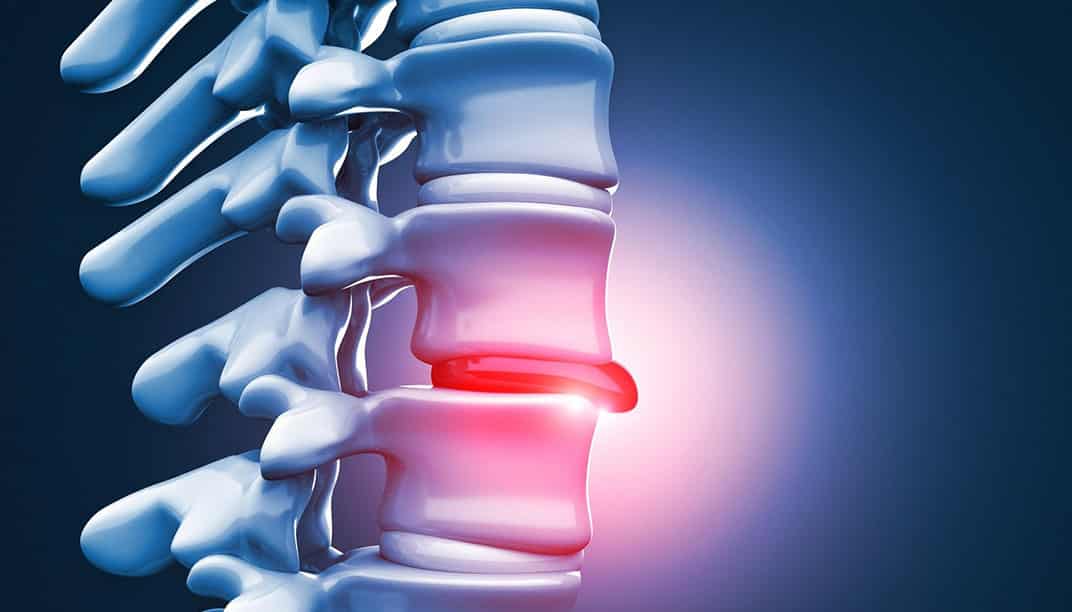
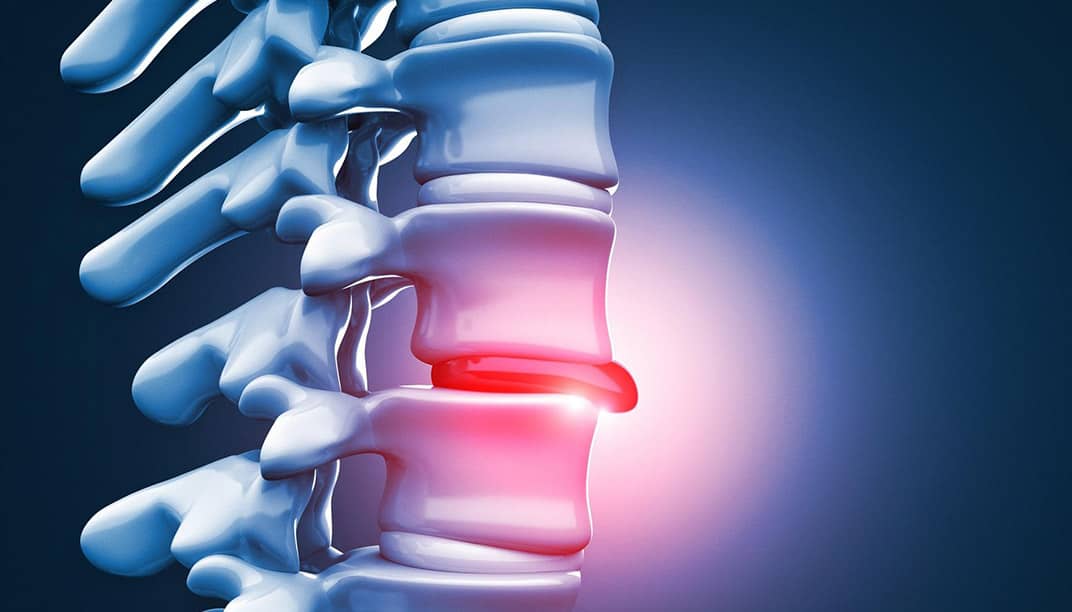
A herniated disc occurs when the soft inner core of a spinal disc pushes through a tear in the outer layer, pressing on nearby nerves. This can happen in two main areas:
- Lumbar disc herniation surgery: In the lower back, causing pain, numbness, or tingling that radiates to the buttocks, thigh, or leg (sciatica).
- Cervical disc herniation surgery: In the neck, leading to pain, weakness, or numbness in the shoulder, arm, or hand.
While both types can be debilitating, the location determines the symptoms and treatment approach.
Types and Common Causes of Disc Herniation
Disc herniation is classified by severity:
- Grade 1: Minor disc bulge
- Grade 2: Moderate protrusion
- Grade 3: Partial disc rupture
- Grade 4: Complete disc rupture with fragment separation
Common causes include age-related degeneration, trauma, repetitive strain, or poor posture. The more severe the herniation, the higher the chance of needing surgical intervention.
When Is Herniated Disc Surgery Necessary?
Symptomatic Herniated Disc with Persistent Neurological Signs
Surgery is typically considered when:
- Pain and neurological symptoms persist despite 6 weeks of conservative treatment
- There is progressive muscle weakness (e.g., foot drop)
- Numbness or tingling is worsening and affecting mobility
These are strong indicators that herniated disc surgery may be necessary.
Symptoms Requiring Herniated Disc Surgery: Cauda Equina, Bladder, or Bowel Dysfunction
Some symptoms signal a medical emergency:
- Loss of bladder or bowel control
- Severe numbness in the saddle area (inner thighs, buttocks, genitals)
- Complete leg weakness or paralysis
These may indicate cauda equina syndrome, a rare but serious condition caused by severe nerve compression. Herniated disc cauda equina surgery must be performed within 24–48 hours to prevent permanent paralysis.
Herniated Disc Surgical Indications
Herniated Disc Surgical Indications in the Lumbar Spine
Surgery is recommended for lumbar herniations when:
- Imaging confirms nerve root compression
- Conservative treatments (medication, physical therapy, injections) have failed
- There is evidence of progressive neurological decline
This is especially true for patients with disabling sciatica or significant functional limitations.
Cervical Disc Herniation Surgery Indications After Failed Conservative Care
For cervical disc herniation, surgery may be needed if:
- Neck pain radiates to the arm with weakness
- Hand coordination is affected
- Conservative care fails after 6–8 weeks
Early intervention can prevent long-term nerve damage.
Herniated Disc Surgery vs Conservative Treatment
When Is Herniated Disc Surgery Necessary Compared to Physical Therapy
Most herniated discs (about 80%) improve with conservative treatment, including:
- Anti-inflammatory medications
- Physical therapy
- Targeted exercises
- Epidural steroid injections
However, if symptoms persist or worsen, herniated disc surgery becomes a necessary step.
Success Rates of Herniated Disc Surgery vs Conservative Treatment
- Conservative treatment success rate: ~70–80% over 6–12 weeks
- Herniated disc surgery success rate: ~90%, with faster pain relief and functional recovery
Surgery is especially effective for patients with clear nerve compression and disabling symptoms.
Types of Herniated Disc Surgery
Overview of Minimally Invasive Herniated Disc Surgery (Endoscopic Discectomy, Microdiscectomy)
- Microdiscectomy: A minimally invasive procedure using a small incision and microscope to remove the herniated portion of the disc. It’s the most common type of herniated disc surgery, with a short recovery time.
- Endoscopic discectomy for a herniated disc: Even less invasive, using a tiny camera and specialized tools. Ideal for selected cases with single-level herniation.
Both techniques aim to relieve nerve pressure with minimal tissue damage.
Conditions Requiring More Extensive Procedures
In advanced cases, additional procedures may be needed:
- Laminectomy: To remove part of the vertebra and relieve nerve pressure
- Spinal fusion: To stabilize the spine after disc removal, especially in cases of instability or multi-level disease
These are reserved for complex or recurrent herniations.
Herniated Disc Surgery Recovery Timeline
Post-Surgery Rehabilitation and Early Recovery
Recovery begins immediately:
- Day 1–2: Walking with assistance, light movement encouraged
- Week 1–2: Gradual increase in walking distance, start of gentle stretching
- Week 3–6: Introduction of core strengthening and balance exercises
This herniated disc surgery timeline supports healing and prevents stiffness.
Long-Term Phases in Herniated Disc Surgery Recovery and Full Recovery Guide
- Month 1–3: Return to light daily activities and sedentary work
- Month 4–6: Resume most normal activities, including light exercise
- After 6 months: Full recovery for most patients, with continued focus on spinal health
The herniated disc full recovery guide emphasizes consistency and long-term care.
Herniated Disc Surgery Risks and Success Rate
Common Herniated Disc Surgery Risks and How to Mitigate Them
Despite high success rates, potential herniated disc surgery risks include:
- Infection at the surgical site
- Deep vein thrombosis (DVT)
- Recurrent disc herniation
- Nerve injury (rare)
To reduce risks:
- Begin early mobilization
- Take prescribed blood thinners
- Follow wound care instructions
- Attend all follow-up visits
Herniated Disc Surgery Success Rate Statistics
The herniated disc surgery success rate is approximately 90%, with most patients reporting significant improvement in pain and function within a few weeks. Long-term outcomes are excellent when combined with proper rehabilitation.
Herniated Disc Recovery Exercises
Essential Herniated Disc Recovery Exercises Post-Surgery
Key herniated disc recovery exercises include:
- Pelvic tilts: Reduce lower back pressure
- Heel slides: Improve flexibility
- Nerve gliding exercises: Relieve numbness and tingling
- Core strengthening (planks, bridges): Support spinal stability
These should be done under the guidance of a physical therapist.
Tips for Safe and Effective Progression
- Start slowly and increase intensity gradually
- Avoid high-impact activities early on
- Maintain proper posture during all movements
- Listen to your body — pain is a warning sign
A structured post-surgery rehabilitation program ensures safe progress.
Full Recovery Guide After Herniated Disc Surgery
Long-Term Outcomes in Herniated Disc Full Recovery Guide
Most patients return to normal life within 6–12 weeks, but full recovery can take up to 6 months. Long-term success depends on:
- Adherence to exercise routines
- Maintaining a healthy weight
- Practicing good posture and body mechanics
Lifestyle Changes and Prevention Strategies Post-Recovery
To prevent recurrence:
- Practice ergonomic habits at work and home
- Engage in regular low-impact exercise (walking, swimming, yoga)
- Strengthen core and back muscles
- Avoid heavy lifting and twisting motions
These habits are essential for lasting spinal health.
Conclusion
If you're suffering from herniated disc symptoms, don’t wait for your condition to worsen. At Safemedigo, we offer accurate diagnosis and comprehensive treatment — whether through conservative care or herniated disc surgery when necessary.
With a personalized herniated disc post-surgery rehabilitation plan and expert medical support, we help you regain mobility and live pain-free.
Don’t hesitate to contact us today to schedule a free consultation and start your journey to recovery.
Frequently Asked Questions: Herniated Disc Surgery: When Is It Necessary? Full Recovery Guide
Can a herniated disc heal without surgery?
Yes, most cases improve with conservative treatment, including physical therapy, medications, and lifestyle changes.
When should surgery be performed?
Surgery is recommended when pain persists beyond 6 weeks or if there are serious neurological symptoms like loss of bladder control.
What’s the difference between lumbar and cervical disc herniation?
Lumbar disc herniation affects the lower back and legs, while cervical disc herniation affects the neck, arms, and hands.
How long is recovery after herniated disc surgery?
Recovery typically takes 6 to 12 weeks, depending on the type of surgery and the patient’s overall health.
Do symptoms return after surgery?
Yes, in some cases, but following a long-term exercise and posture correction plan greatly reduces the risk of recurrent herniated disc.