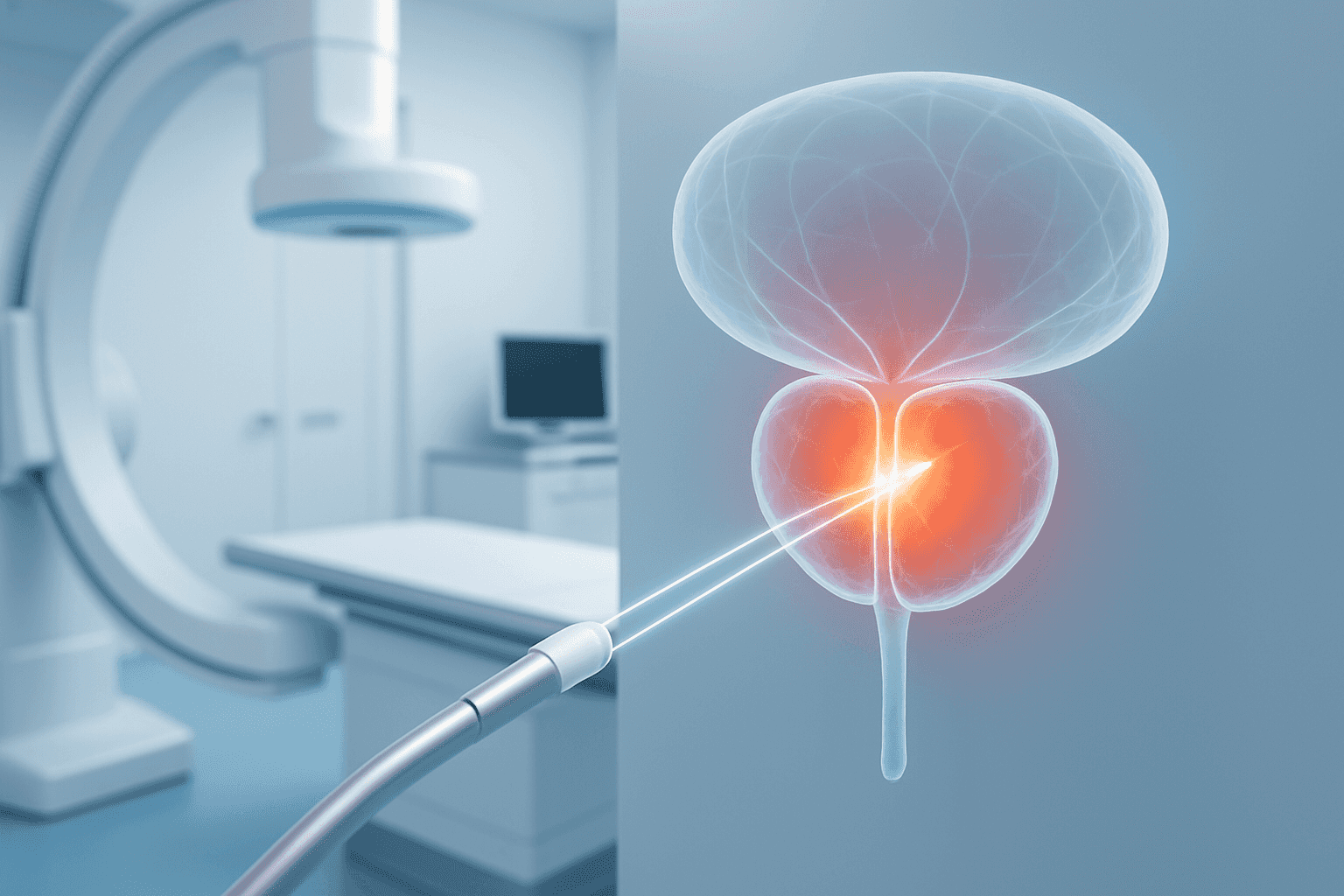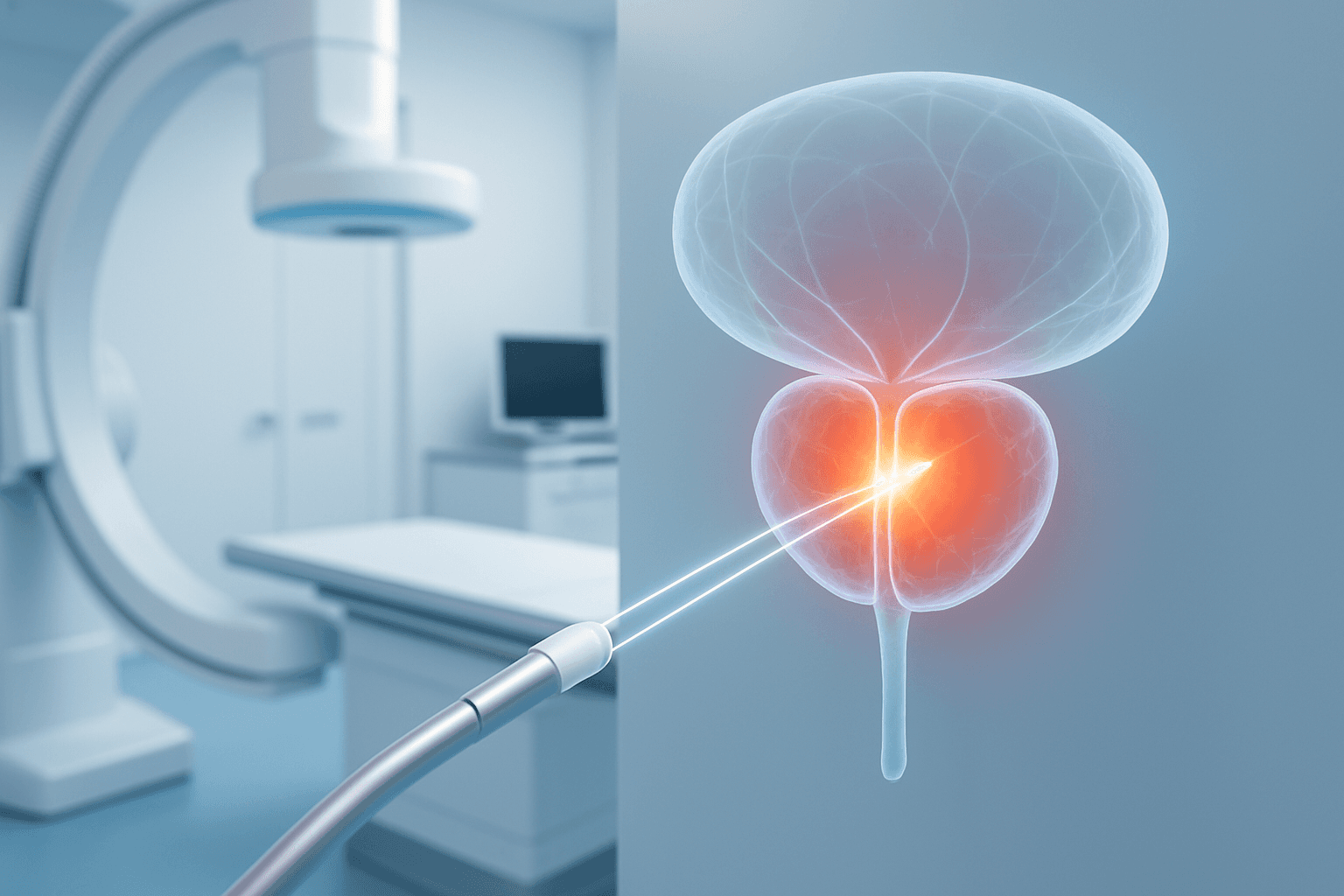
The field of oncology is undergoing a tremendous evolution, especially concerning prostate cancer, one of the most common cancers among men. In the past, treatment options were often limited to radical surgery or external beam radiation, procedures that carry significant side effects that can impact a patient's quality of life. This reality has driven the medical community to search for more precise and less invasive alternatives.
With the dawn of modern medicine, interventional radiology has emerged as one of the most prominent innovations that has changed the game. This technology represents a true revolution in prostate cancer treatment, offering targeted solutions that directly attack the tumor with minimal damage to surrounding healthy tissue. This approach not only promises high efficacy in eliminating cancer cells but also helps reduce complications and improve the overall patient experience.
In this comprehensive guide, we will explore the world of interventional radiology for prostate cancer and review the latest available techniques, from thermal and radiofrequency ablation to focal therapy. At Safemedigo, we believe in the importance of empowering patients with knowledge, and through this article, we aim to highlight these advanced options to help you understand how modern medicine can provide you with the best possible care.
What Is Interventional Radiology Prostate Cancer Treatment?
To understand the true value of this therapeutic revolution, we must first delve into the concept of interventional radiology and how it differs from traditional approaches.
Definition of interventional radiology prostate cancer techniques
Interventional radiology is a modern medical specialty that combines advanced imaging techniques (such as ultrasound, CT scans, and MRI) with minimally invasive procedures. In the context of prostate cancer treatment, doctors use these techniques to guide precise instruments, like needles or catheters, directly to the tumor within the prostate through very small incisions, no larger than a few millimeters. This allows for the application of localized prostate cancer treatment with pinpoint accuracy.
Difference between interventional radiology and traditional treatment
The fundamental difference lies in the level of invasiveness. Traditional surgery requires a large incision and removal of the entire prostate, which increases the risk of complications such as urinary incontinence and erectile dysfunction. External beam radiation directs radiation from outside the body, which can affect adjacent healthy tissues. In contrast, minimally invasive prostate cancer treatment is a targeted approach that treats the tumor from the inside, preserving as much healthy tissue as possible.
Why is the latest prostate cancer treatment using interventional radiology advancing rapidly
This approach has become an advanced option because it offers a perfect balance between efficacy and safety. It allows for the destruction of tumors with high precision, significantly reduces recovery time, and lowers the rates of complications associated with traditional treatments. This makes it an ideal choice for many patients, especially those with early prostate cancer or those who cannot tolerate major surgery.
Read about: Interventional Radiology for Enlarged Prostate Treatment
Latest Prostate Cancer Treatment Using Minimally Invasive Techniques
There are multiple techniques used within the framework of interventional radiology, each employing a different mechanism to destroy cancer cells.
Prostate cancer radiofrequency ablation explained
Prostate cancer radiofrequency ablation (RFA) involves inserting a fine needle into the tumor, which emits radiofrequency waves. These waves generate high heat that effectively heats and destroys cancer cells. This technique is an excellent option for small, well-defined tumors.
How prostate cancer microwave ablation works
Prostate cancer microwave ablation (MWA) uses microwave energy to generate rapid and intense heat within the tumor. This technique is capable of treating larger tumors more quickly compared to radiofrequency ablation, making it a promising option in certain cases. To get a consultation on the most suitable technique for your condition, you can contact the Safemedigo team via WhatsApp.
Focal therapy for prostate cancer as a modern approach
Focal therapy for prostate cancer represents a paradigm shift from "whole-gland treatment" to "tumor-only treatment." It involves various techniques, including cryotherapy, HIFU, and thermal ablation, all aimed at destroying only the cancerous part of the prostate while preserving the rest of the gland and its functions.
Prostate Cancer Catheter Treatment and Image-Guided Procedures
Catheters and micro-instruments are the cornerstones of these advanced treatments, allowing access to the deepest areas with minimal intervention.
Role of prostate artery embolization in tumor management
In some cases, particularly for advanced prostate cancer treatment, prostate artery embolization (PAE) can be used. A microcatheter is inserted through an artery in the groin and guided to the arteries supplying the tumor. Tiny particles are then injected to block these arteries, cutting off the blood supply to the tumor and causing it to shrink and die. This is also known as prostate cancer catheter treatment.
Image-guided prostate cancer treatment for precision targeting
The essence of the success of these techniques is precision. Using real-time imaging, the physician can see the needle or catheter as it enters the body and reaches the tumor with millimeter accuracy. This image-guided prostate cancer treatment ensures that the therapy is concentrated exactly where it needs to be, maximizing its effectiveness and minimizing collateral damage.
Prostate cancer ablation using thermal and advanced energy sources
Prostate cancer ablation is another term describing thermal treatments like radiofrequency and microwave ablation. The idea is to "ablate" or burn the tumor from the inside with extreme precision, ensuring the destruction of cancer cells without the need for surgical removal. This reduces surgical trauma and speeds up the healing process.
Read about: Latest Non-Surgical Treatments for Enlarged Prostate
Localized Prostate Cancer Treatment Using Ablation Technologies
Localized treatment represents a paradigm shift from treating the entire gland to treating only the tumor, a concept known as focal therapy.
Prostate cancer cryotherapy as a focal treatment option
Prostate cancer cryotherapy involves freezing the tumor to destroy it. It is a form of focal therapy where probes are inserted into the prostate to deliver extremely cold gases, creating an ice ball that engulfs and kills the cancer cells. This technique is highly effective for localized tumors.
Effectiveness of localized prostate cancer treatment in early stages
Studies have shown that localized prostate cancer treatment is highly effective in controlling early-stage, organ-confined prostate cancer. It offers cure rates comparable to traditional surgery or radiation in carefully selected cases, but with significantly fewer side effects related to urinary and sexual function.
Comparison between prostate cancer ablation and surgical removal
Traditional surgery removes the entire prostate, which ensures cancer removal but at the cost of an increased risk of complications. Prostate cancer ablation, on the other hand, focuses only on the tumor, significantly reducing these risks. However, ablation may require careful follow-up to ensure the cancer does not recur in other parts of the gland.
Non-Surgical Prostate Cancer Treatment Options
The appeal of these techniques lies in the numerous benefits they offer compared to open surgery.
Benefits of minimally invasive prostate cancer treatment
The main benefits include a shorter hospital stay, faster recovery, less pain, minimal scarring, and a significantly lower risk of major complications. This non-surgical prostate cancer treatment approach helps patients return to their normal lives much more quickly.
Recovery time after interventional radiology prostate cancer procedures
Because the procedure is performed through tiny incisions, the recovery time is remarkably fast. Most patients can go home the same or the next day and resume their normal activities within a few days, compared to weeks or months after traditional surgery.
Avoiding complications of traditional prostate cancer surgery
The biggest advantage is the preservation of vital functions. These treatments significantly reduce the risks of permanent urinary incontinence and erectile dysfunction, two of the most feared complications after radical prostatectomy. This preservation of quality of life is a key reason why patients prefer these options.
Early and Advanced Prostate Cancer Treatment Approaches
These treatments are suitable for a wide range of patients, but the choice depends on the tumor stage and the patient's health status.
Early prostate cancer treatment with modern technologies
Patients with early prostate cancer that is still confined within the gland are the ideal candidates for these techniques. At this stage, focal therapy can completely eradicate the tumor while preserving the rest of the gland, offering a chance for a complete cure with minimal side effects.
Advanced prostate cancer treatment using interventional radiology
Even in cases of advanced tumors that have spread beyond the prostate, interventional radiology can play an important role. It can be used as a palliative treatment to relieve pain from bone metastases or to reduce the size of the main tumor to alleviate urinary symptoms, thereby improving the patient's quality of life.
When targeted prostate cancer therapy becomes necessary
Targeted prostate cancer therapy is crucial when the goal is to treat the cancer effectively while minimizing harm to the body. It becomes necessary for patients who are poor surgical candidates, have a strong desire to preserve sexual and urinary function, or have recurrent cancer after previous treatments.
Read about: Prostate Enlargement Treatments: Medication or Surgery
Who Can Benefit From Modern Prostate Cancer Therapy?
These treatments are suitable for a wide range of patients, but the selection depends on the stage of the tumor and the patient's overall health.
Suitability of focal therapy for prostate cancer patients
Patients with localized, clinically significant prostate cancer that is visible on MRI are excellent candidates for focal therapy. It is an ideal option for men who want to avoid the side effects of radical treatments. To discuss your case with experts, contact the experts at Safemedigo today.
Patients who benefit from non-surgical prostate cancer treatment
Patients who are older, have other significant health problems, or simply wish to avoid surgery can greatly benefit from these non-surgical options. They offer a less stressful and physically demanding alternative to traditional surgery.
Selecting between ablation, embolization, and catheter-based procedures
The choice of a specific modern prostate cancer therapy depends on tumor size, location, and stage, as well as the patient's overall health and preferences. A multidisciplinary team of experts is best suited to recommend the most appropriate procedure for each individual case.
Conclusion
Ultimately, the emergence of interventional radiology as the latest prostate cancer treatment marks a milestone in modern medicine. These techniques have ushered in a new era of precise, personalized therapies that prioritize the patient's quality of life alongside efficacy in fighting the disease.
Patients no longer have to choose between curing their cancer and preserving their vital functions. Minimally invasive treatments offer an ideal compromise, providing tumor control while significantly reducing risks and complications. The choice among these techniques depends on a thorough evaluation of the case by a multidisciplinary medical team.
If you or a loved one is facing a prostate cancer diagnosis, knowledge is your most powerful weapon. Contact the Safemedigo team today via WhatsApp to explore how the latest prostate cancer treatments using interventional radiology can offer you hope and healing. Let our experts guide you toward the best option for your health and your future.
Frequently Asked Questions: Latest Prostate Cancer Treatment Using Interventional Radiology
Are these treatments painful?
Most of these procedures are performed under local anesthesia with intravenous sedation or light general anesthesia. Patients feel minimal pain during the procedure, and any subsequent discomfort can be easily managed with simple pain relievers.
How long does the procedure take?
Most interventional radiology procedures for prostate cancer take between one to three hours, depending on the size and complexity of the tumor and the technique used.
Can the cancer come back after focal therapy?
Yes, there is a possibility of cancer recurrence in another, untreated part of the prostate. For this reason, regular, diligent follow-up with your doctor, including blood tests (PSA) and MRI scans, is an essential part of the long-term treatment plan.
What is the difference between cryotherapy and thermal therapy?
Both are focal ablation techniques, but they use opposite mechanisms. Cryotherapy uses extreme cold to freeze and destroy cancer cells, while thermal therapy (like radiofrequency ablation) uses high heat to burn them. The choice between them depends on the tumor's location and the physician's preference.