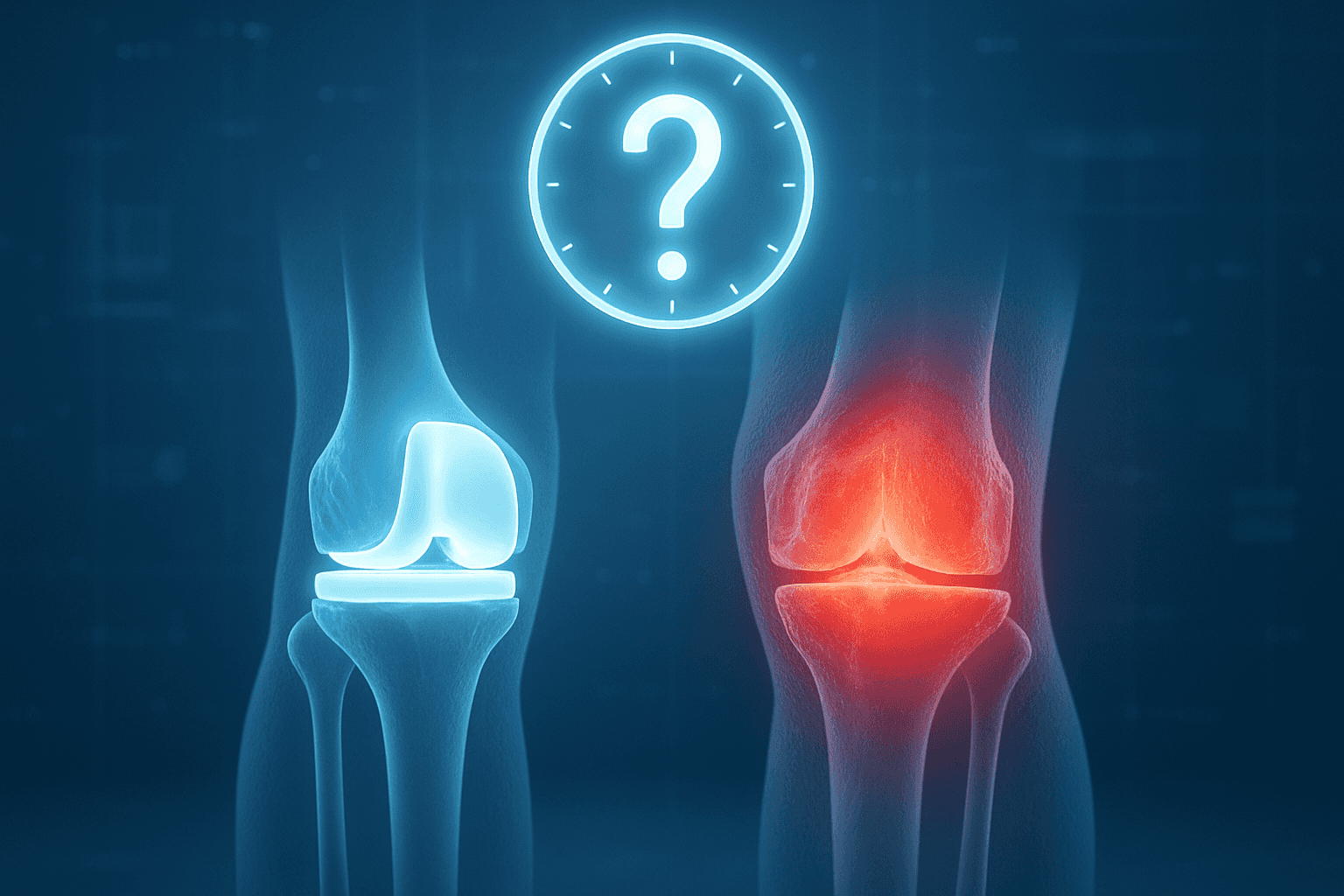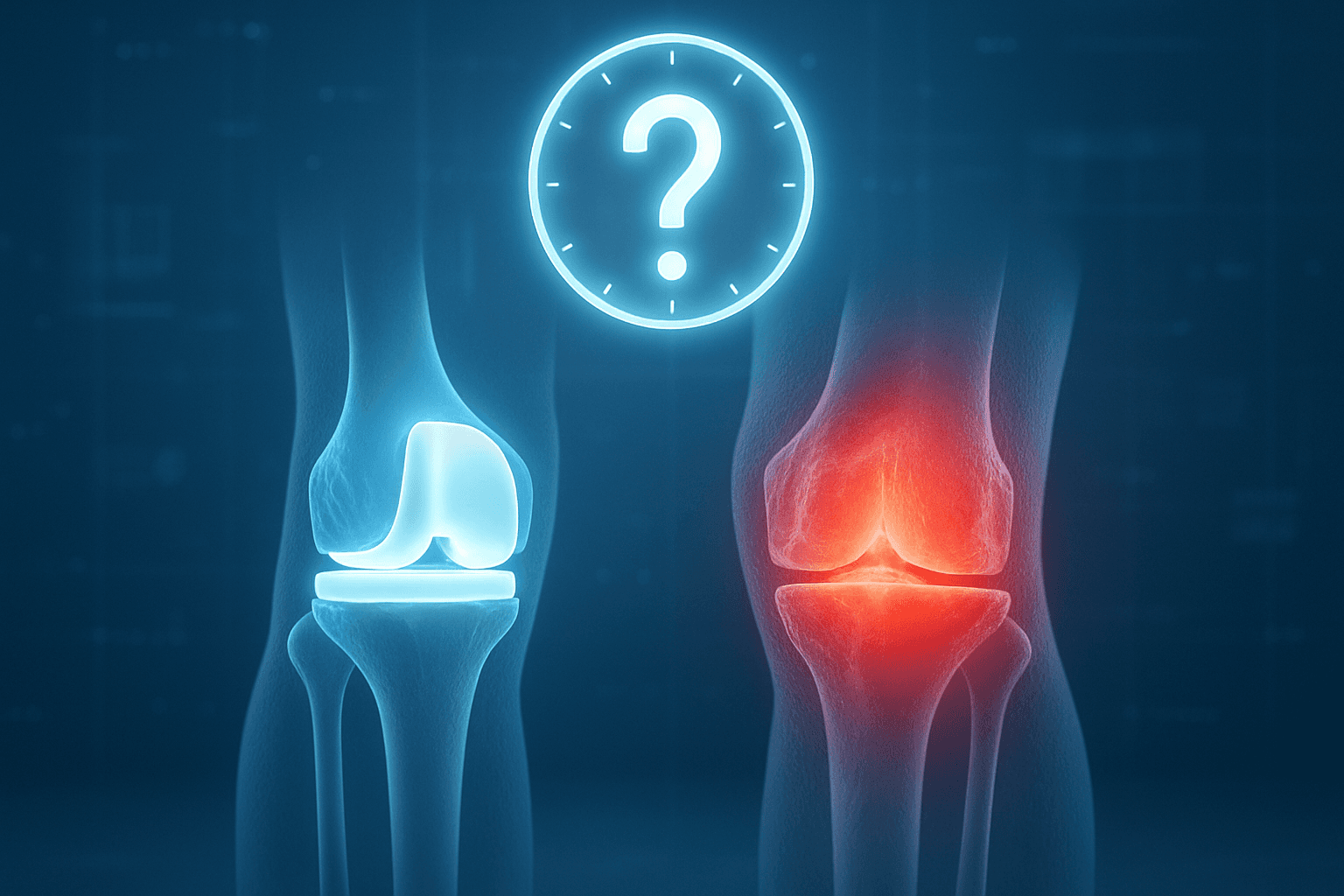
Chronic knee pain is one of the most common health issues affecting the quality of life for millions worldwide, limiting their ability to move and turning the simplest daily activities into significant challenges. When conservative treatments like medication and physical therapy fail to provide adequate relief, knee joint replacement emerges as a radical and effective solution to restore movement and eliminate pain.
Deciding to undergo knee replacement surgery is not an easy step. It requires a deep understanding of the medical condition, precise knowledge of the indications for the procedure, its timing, and full awareness of the expected benefits and potential risks. This decision represents a turning point in a patient's life, promising a more active and free future.
In this comprehensive guide, we will extensively explain everything related to knee joint replacement surgery, from its definition and components to the reasons for choosing it, and the details of the procedure and subsequent rehabilitation. At Safemedigo, we aim to provide you with all the information you need to make an informed decision about your health and your future mobility.
What Is Knee Joint Replacement Surgery?
Knee joint replacement is an advanced surgical procedure aimed at restoring the function of a severely damaged knee, and it stands as one of the most successful surgical operations in modern medical history.
Definition of knee joint replacement
Knee joint replacement, medically known as "knee arthroplasty," is a surgical procedure in which the damaged joint surfaces of the knee bones (femur, tibia, and patella) are removed and replaced with artificial parts made of highly durable materials such as metals and strong plastic polymers. The primary goal of this procedure is to alleviate severe pain that does not respond to other treatments, correct deformities, and restore the ability to move and perform daily functions normally.
How knee replacement surgery works
A typical artificial knee joint consists of several parts that precisely mimic the function of the natural joint. These components are:
- Femoral Component: This is a polished metal part that is fixed to the end of the femur (thigh bone). This component takes the shape of the natural end of the bone and allows for smooth gliding movement.
- Tibial Component: This is a flat part that is fixed to the top of the tibia (shin bone). It usually consists of a metal base and a plastic upper surface.
- Polyethylene Insert: This is a piece of high-density medical-grade plastic (polyethylene) placed between the femoral and tibial components. This insert acts as an artificial cartilage surface, reducing friction and allowing for smooth gliding between the two metal parts.
- Patellar Component: In some cases, the back surface of the patella (kneecap) is also replaced with a dome-shaped plastic piece. This procedure is not always necessary and depends on the condition of the patella.
These components work together to provide a stable and smooth joint, allowing the patient to bend and extend the knee without pain, thus restoring the ability to walk, climb stairs, and perform other activities.
When doctors recommend knee joint replacement
A doctor begins to seriously consider knee joint replacement surgery when the patient's condition reaches an advanced stage of deterioration and conservative treatments are no longer sufficient to control the symptoms. This decision is based on a range of factors, not just radiographic images. The doctor considers this option when the patient suffers from severe and persistent pain that interferes with sleep and rest, when walking short distances or climbing stairs becomes extremely painful, and when the condition negatively affects the patient's overall quality of life, preventing them from enjoying their hobbies or performing their daily tasks.
Why Do You Need Knee Replacement Surgery?
The need for knee replacement surgery arises from the deterioration of the joint to a degree where pain and disability become an integral part of the patient's daily life.
Common reasons for knee joint replacement
The most common reasons leading to the need for a knee replacement are diseases that cause the erosion of the articular cartilage. The most prominent of these indicators are:
- Osteoarthritis: This is the most common cause, known as "wear-and-tear arthritis." It occurs as a result of the gradual erosion of the cartilage that covers the ends of the bones with age or due to overuse, leading to the bones rubbing against each other, causing pain and stiffness.
- Rheumatoid Arthritis: This is an autoimmune disease in which the immune system attacks the synovial membrane of the joint, causing chronic inflammation that leads to the destruction of cartilage and bone.
- Post-traumatic Arthritis: This type of arthritis can occur years after a serious knee injury, such as a fracture of the bones surrounding the knee or a ligament tear, which alters the mechanics of the joint and leads to cartilage wear.
Symptoms that indicate you need knee replacement
A patient needs a knee replacement when the symptoms become so severe that they significantly disrupt their life. The decision is not based on a single factor but on a comprehensive assessment of the condition. Generally, a patient becomes a strong candidate for the surgery when they experience severe knee pain at rest, day or night, or pain that prevents them from sleeping. Also, when pain and stiffness become an obstacle to performing simple activities like getting up from a chair, walking, or using stairs. In addition, if painkillers or anti-inflammatory drugs are no longer effective, or if they cause unbearable side effects, surgical intervention becomes a necessary option.
Benefits of knee joint replacement for mobility
The greatest benefit of knee joint replacement surgery is the elimination of chronic pain, which directly translates into a significant improvement in mobility. After the rehabilitation period, most patients are able to regain a near-normal range of motion in the knee, allowing them to return to activities they had given up for years. Benefits include improved ability to walk longer distances without pain, easier climbing and descending of stairs, and the ability to engage in light recreational activities such as swimming and cycling. This improvement in mobility not only enhances physical independence but also improves the patient's mental and psychological health.
When to Opt for Knee Replacement Surgery
Choosing the right time to have the surgery is one of the most important decisions a patient makes in consultation with their doctor, as it significantly affects the outcome of the operation.
Signs you need knee replacement surgery
The decision to have surgery is not based on the patient's age or the degree of wear on the X-ray alone, but primarily on the degree of pain and disability. Signs that it might be time to make the decision include:
- Unbearable Pain: When the pain becomes so severe that it wakes you up from sleep or prevents you from doing your favorite activities.
- Failure of Conservative Treatments: When painkillers, cortisone injections, physical therapy, or the use of a cane no longer provide sufficient relief.
- Functional Decline: When you find it extremely difficult to walk, get up from a seat, or put on your clothes and socks.
- Obvious Deformities: When the knee begins to bend noticeably inward or outward (bow-legged or knock-kneed).
When conservative treatments no longer help
There is a common misconception that a patient should wait until the pain is "absolutely unbearable" before having surgery. However, delaying the surgery for too long can lead to less than optimal results. When a patient waits too long, complications such as severe weakness in the muscles surrounding the knee, severe joint stiffness, and a decline in general health due to lack of movement can occur. All these factors can make the recovery process after surgery more difficult and longer. Therefore, the optimal timing is when the pain and disability are significant, but the patient is still in good general health and has enough muscle strength to successfully support the rehabilitation process.
How to decide the right time for knee joint replacement
The doctor conducts a comprehensive evaluation to determine if the time is right for surgery. This evaluation includes:
- Detailed Medical History: The doctor listens carefully to the patient's description of the pain, how it affects their daily life, and what treatments they have tried.
- Physical Examination: The doctor examines the knee to assess the range of motion, stability, muscle strength, and degree of deformity.
- X-rays: X-rays show the extent of cartilage wear, joint space narrowing, and the presence of bone spurs.
- Quality of Life Assessment: Doctors sometimes use standardized questionnaires to objectively assess the impact of knee pain on the patient's quality of life.
Based on all this information, the doctor discusses the pros and cons of surgery at this specific time with the patient, helping them make the best decision for their situation. If you are suffering from knee pain and looking for an accurate assessment, you can contact the team of experts at Safemedigo for a specialized consultation.
Types of Knee Joint Replacement
There is no one-size-fits-all type of knee joint. The choice of the appropriate joint depends on several factors, including the extent of damage to the knee, the patient's age, and their activity level.
Total knee replacement vs partial knee replacement
The decision between a total and partial replacement depends on the location and extent of cartilage wear in the knee. The knee is divided into three main compartments: the medial (inner) compartment, the lateral (outer) compartment, and the patellofemoral (between the kneecap and the femur) compartment.
- Total Knee Replacement (TKR): This is the most common procedure, in which the surfaces of all three compartments are replaced. It is resorted to when the wear is widespread in most parts of the knee.
- Partial Knee Replacement (PKR): Also known as unicompartmental replacement, this procedure involves replacing only one part of the knee (usually the medial compartment). This procedure is chosen when the damage is confined to a single compartment, and the surrounding ligaments are intact. This procedure is characterized by a smaller surgical incision, less blood loss, and a faster recovery period compared to total replacement.
Best knee implant options
Implant designs have evolved significantly to meet the needs of different groups. The "best" implant is the one that fits the patient's anatomy and lifestyle.
- For older, less active patients: A traditional posterior-stabilized implant may be an excellent choice. This design provides good stability and high long-term reliability.
- For younger, more active patients: The surgeon may recommend newer designs, such as cruciate-retaining implants that allow for more natural movement, or implants made of more wear-resistant materials like oxidized zirconium (Oxinium) or highly cross-linked polyethylene, which are expected to last longer.
Knee joint replacement for arthritis patients
For patients suffering from rheumatoid arthritis or other types of inflammatory arthritis, knee replacement surgery is often the optimal solution to relieve pain and restore function. In these cases, a total knee replacement is usually the preferred option, as the inflammation tends to affect all parts of the joint equally. The inflammatory condition must be well-managed with appropriate medications before and after surgery to ensure the best results and reduce the risk of complications such as infection.
Read about: Top Knee Replacement Technologies Available in Turkey
Knee Replacement Surgery Procedure
Good preparation for the surgery and understanding what will happen during and after it helps to reduce anxiety and ensure a smooth and successful recovery.
Preparing for knee joint replacement surgery
Preparation begins weeks before the surgery. The medical team will conduct a comprehensive health assessment to ensure you are fit for the operation. This may include blood tests, an electrocardiogram (ECG), and a chest X-ray. It is important to inform the surgeon of all medications and supplements you are taking. You may be asked to stop taking some medications, such as blood thinners, before the surgery. It is strongly recommended to quit smoking, as it slows healing and increases the risk of complications. Also, doing some exercises to strengthen the thigh and arm muscles before surgery can greatly facilitate the recovery process.
Steps during the knee replacement operation
The operation usually takes one to two hours. After anesthesia (either general or spinal), the surgeon performs the following steps:
- Making an incision: The surgeon makes an incision on the front of the knee to access the joint.
- Removing the damaged surfaces: Using precise instruments, the surgeon removes the worn-out parts of the cartilage and bone from the end of the femur and the top of the tibia.
- Positioning the implants: The pre-selected metal and plastic components are fitted and secured in place using a special adhesive called "bone cement" or through a "press-fit" technique that allows the bone to grow into and bond with the implant.
- Closing the incision: After ensuring that the joint is functioning correctly and is stable, the surgeon closes the incision with sutures or surgical staples.
Post-surgery rehabilitation and physical therapy
Rehabilitation begins on the same day as the surgery or the day after. A physical therapist will help you stand and walk using a walker or crutches. The goal of early rehabilitation is to restore movement and prevent blood clots. The rehabilitation program includes exercises to strengthen the muscles around the knee and increase its range of motion. This program continues for several weeks or months after the surgery and is an integral part of the success of the operation. Adherence to the physical therapy program is the key to returning to an active and normal life.
Read about: Knee Joint Replacement Rehab: Steps and Pain Management
Benefits and Risks of Knee Joint Replacement
Like any major surgical procedure, knee replacement surgery carries significant benefits but is not without some potential risks that the patient should be aware of.
Advantages of knee joint replacement surgery
The benefits outweigh the risks for most patients. The most prominent benefit is significant pain relief or complete elimination of pain, which allows patients to sleep better and live more comfortably. The second benefit is the restoration of function and mobility, enabling patients to return to their daily and recreational activities. This improvement in independence has a huge positive impact on mental health and self-confidence, leading to an overall improvement in quality of life.
Possible knee replacement complications
Although the success rate of the operation is very high, there are some potential complications, albeit rare. These complications include:
- Infection: This is one of the most serious complications. A superficial infection can occur in the wound, or a deep infection can occur around the implant. Strict preventive measures are taken to reduce this risk, such as administering antibiotics before and after surgery.
- Blood Clots: Clots can form in the leg veins (DVT) after surgery and can travel to the lungs (PE), causing a serious condition. Blood thinners are given, compression stockings are used, and early movement is encouraged to prevent this.
- Implant Wear or Loosening: Over time, the plastic components of the joint may wear out, or the implant may loosen from the bone.
- Knee Stiffness: Some patients may not be able to regain the full range of motion, especially if they do not adhere to the physical therapy program.
How to minimize surgery risks
To minimize risks, it is crucial to choose an experienced surgeon and a reputable hospital. Following all pre-operative instructions, such as quitting smoking and managing chronic conditions like diabetes, is vital. Post-operatively, strict adherence to the rehabilitation program, wound care, and medication schedule is essential. Being aware of the warning signs of complications and contacting your doctor immediately if they occur can prevent serious problems.
Knee Implant Lifespan and Durability
One of the most common questions patients ask is, "How long will my new joint last?" The answer depends on several factors.
How long does a knee implant last?
Thanks to advances in materials and surgical designs, modern artificial joints have become extremely durable. Long-term studies indicate that “more than 82% of knee replacements are still functioning well after 25 years”. For most patients, a knee replacement can be considered a permanent solution that provides comfort and function for the rest of their lives.
Factors affecting knee replacement longevity
Several factors can affect how long an implant lasts, including:
- Activity Level: Patients who engage in high-impact activities such as running or jumping may subject their implant to faster wear.
- Patient's Weight: Excess weight puts additional stress on the implant, which can accelerate its wear. Maintaining a healthy weight is one of the most important factors in prolonging the life of the joint.
- Patient's Age at Surgery: Younger, more active patients may need revision surgery in the future simply because they will live longer with the implant.
- Surgical Accuracy: The surgeon's skill and precision in placing the implant components play a crucial role in determining its longevity.
Tips to extend the life of a knee implant
To get the most out of your new joint and ensure it lasts as long as possible, follow these tips:
- Maintain a healthy weight: This is the most important thing you can do.
- Avoid high-impact activities: Replace running and sports that require jumping with low-impact activities such as swimming, cycling, and walking.
- Adhere to regular follow-ups: Visit your surgeon regularly for periodic check-ups to ensure everything is fine.
- Prevent infections: Take care of your general health and dental health, and always inform doctors that you have an implant before any medical procedure.
Cost of Knee Joint Replacement Surgery
Cost is an important factor when considering knee replacement surgery. Costs vary significantly depending on the country, hospital, and type of implant used.
Average knee replacement surgery cost
The cost of knee replacement surgery varies widely. In some countries with high medical costs, the operation can be very expensive. In contrast, other countries like Turkey offer high-quality medical care at very competitive prices, making them an attractive destination for medical tourism. When comparing costs, it is important to look at the overall value, which includes the surgeon's experience, the quality of the hospital, and the type of implant used.
What affects the total cost of knee surgery
The total cost of the operation is usually a package that includes several components:
- The cost of the implant itself: This varies depending on its type and the material it is made of.
- The fees of the surgeon and the anesthesia team.
- Hospital costs: This includes the hospital stay, use of the operating room, medications, and tests.
- Rehabilitation costs: This includes physical therapy sessions during the hospital stay and after discharge.
It is important to get a detailed and clear price quote that specifies all these items to avoid any unexpected costs. At Safemedigo, we offer comprehensive and transparent packages that cover all aspects of your treatment journey.
Insurance coverage for knee joint replacement
Knee replacement surgery is often considered a medically necessary procedure to treat severe pain or joint degeneration. Therefore, most health insurance plans cover it after certain conditions are met, such as exhausting conservative treatments first. It is important to contact your insurance provider before the surgery to obtain prior approval and understand the coverage limits, including costs for surgery, hospital stay, medications, and any portion you may need to pay out of pocket.
Recovery and Aftercare After Knee Replacement
The success of the operation does not end upon leaving the operating room but depends heavily on the patient's adherence to instructions during the recovery period and beyond.
Post-knee replacement care and exercises
In the first few weeks after surgery, you will need to make some adjustments in your home to facilitate movement, such as removing rugs that could cause tripping, using a high chair, and installing grab bars in the bathroom. Continue to use a walker or crutches as directed by your doctor. Listen to your body and avoid over-activity. You can gradually return to your daily activities such as driving and work after consulting your surgeon.
Lifestyle tips after knee replacement surgery
Movement is beneficial, but the right type of exercise must be chosen. Low-impact activities are best for preserving your joint. Excellent options include:
- Walking: This is the best exercise after surgery.
- Swimming and water aerobics: Excellent because the water supports body weight and reduces pressure on the joint.
- Cycling (stationary or outdoors): Helps to strengthen muscles and improve range of motion.
- Golf and dancing.
Sports that involve running, jumping, sudden twisting, and physical contact should be avoided.
Read about: Home Exercises After Knee Replacement Surgery Recovery
When to contact your doctor after surgery
You should contact your doctor immediately if you notice any of the following warning signs, which may indicate a complication:
- Fever or chills.
- Increased redness, swelling, or pain in the knee.
- Any drainage or pus from the wound.
- Pain in the calf or sudden swelling in the leg (may indicate a blood clot).
- Sudden shortness of breath or chest pain (may indicate a pulmonary embolism).
Early intervention in case of any of these symptoms is crucial to ensure your safety and the success of the operation.
Conclusion
Knee joint replacement represents an effective and reliable solution for people suffering from excruciating knee pain and functional decline due to arthritis or injury. The decision to undergo this operation is a big step towards regaining an active, pain-free life. By understanding when the time is right for surgery, choosing the right type of implant, and committing to a comprehensive rehabilitation program, you can achieve excellent results that last for many years.
Success in this journey depends on a strong partnership between you and your medical team. Knowledge and good preparation are the keys to confidence and success. Don't let knee pain control your life anymore.
Frequently Asked Questions: Knee Joint Replacement
What is the best age to have a knee replacement?
There is no specific "ideal age." In the past, it was thought that the surgery should be delayed as long as possible, but with the improved durability of implants, the focus is now on the patient's quality of life. The surgery is successfully performed on patients of various ages, from young people in their forties to seniors in their eighties. The decision depends on the degree of pain and disability, not on chronological age.
Will I be able to kneel or sit on the floor after the surgery?
The ability to kneel or sit on the floor varies from patient to patient. Many patients find it difficult or uncomfortable to kneel directly on the artificial knee. However, with intensive physical therapy and modern implant designs, some patients are able to achieve this. It is best to discuss this with your surgeon and physical therapist.
When can I return to work after knee replacement surgery?
This largely depends on the nature of your job. If you have a desk job that requires sitting most of the time, you may be able to return within 4 to 6 weeks. However, if your job requires standing for long periods, walking, or lifting heavy objects, you may need a longer recovery period of 3 to 6 months.
Will my artificial joint make a noise when I move?
Yes, this is common and not a cause for concern in most cases. Some patients may hear a slight "clicking" or "popping" sound when moving the knee, especially in the first few months after surgery. This sound is caused by the metal and plastic components moving against each other. As long as this sound is not accompanied by pain, there is no need to worry.
Will I need a blood transfusion during or after the surgery?
In the past, blood transfusions were more common. Today, with modern surgical techniques and the use of medications that help reduce bleeding (such as tranexamic acid), the need for a blood transfusion is much lower. Your medical team will assess your condition and determine if you are at risk of significant blood loss.